Venous Ulcer Treatment in Mohali - Expert Vascular Care
A venous leg ulcer (VLU) is one of the most distressing consequences of untreated venous disease — a chronic, open wound on the lower leg that refuses to heal for weeks, months, or even years. Living with a non-healing wound affects mobility, confidence, and everyday quality of life.
Yet despite how common these wounds are, many patients spend months on dressings alone, never receiving treatment for the underlying venous insufficiency driving the problem. Without addressing the root cause, ulcers repeatedly return - making specialist vascular intervention critically important.
"At Fortis Hospital Mohali, patients have access to one of the most experienced vascular surgery teams in North India - treating both the wound and the diseased vein causing it. Heading this programme is Dr. Ravul Jindal, Director & HOD of Vascular Surgery at Fortis Hospital Mohali, with 30+ years of experience and advanced international training at St Mary's Hospital, London, affiliated to Imperial College."
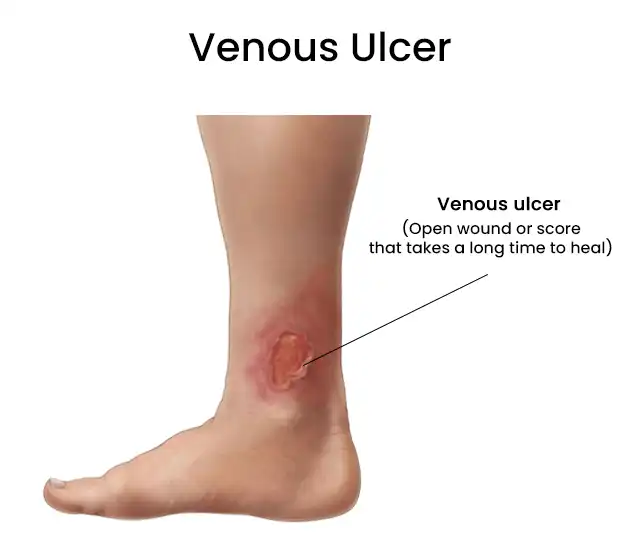
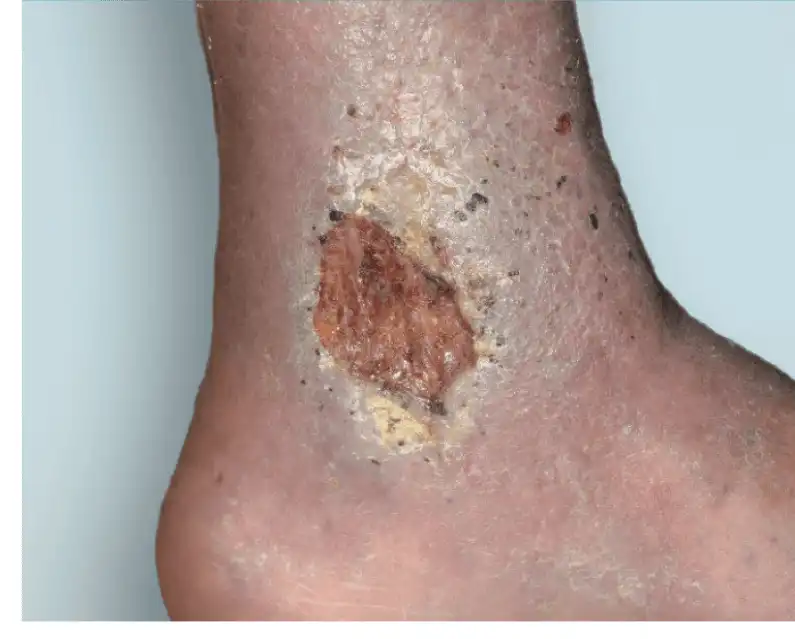
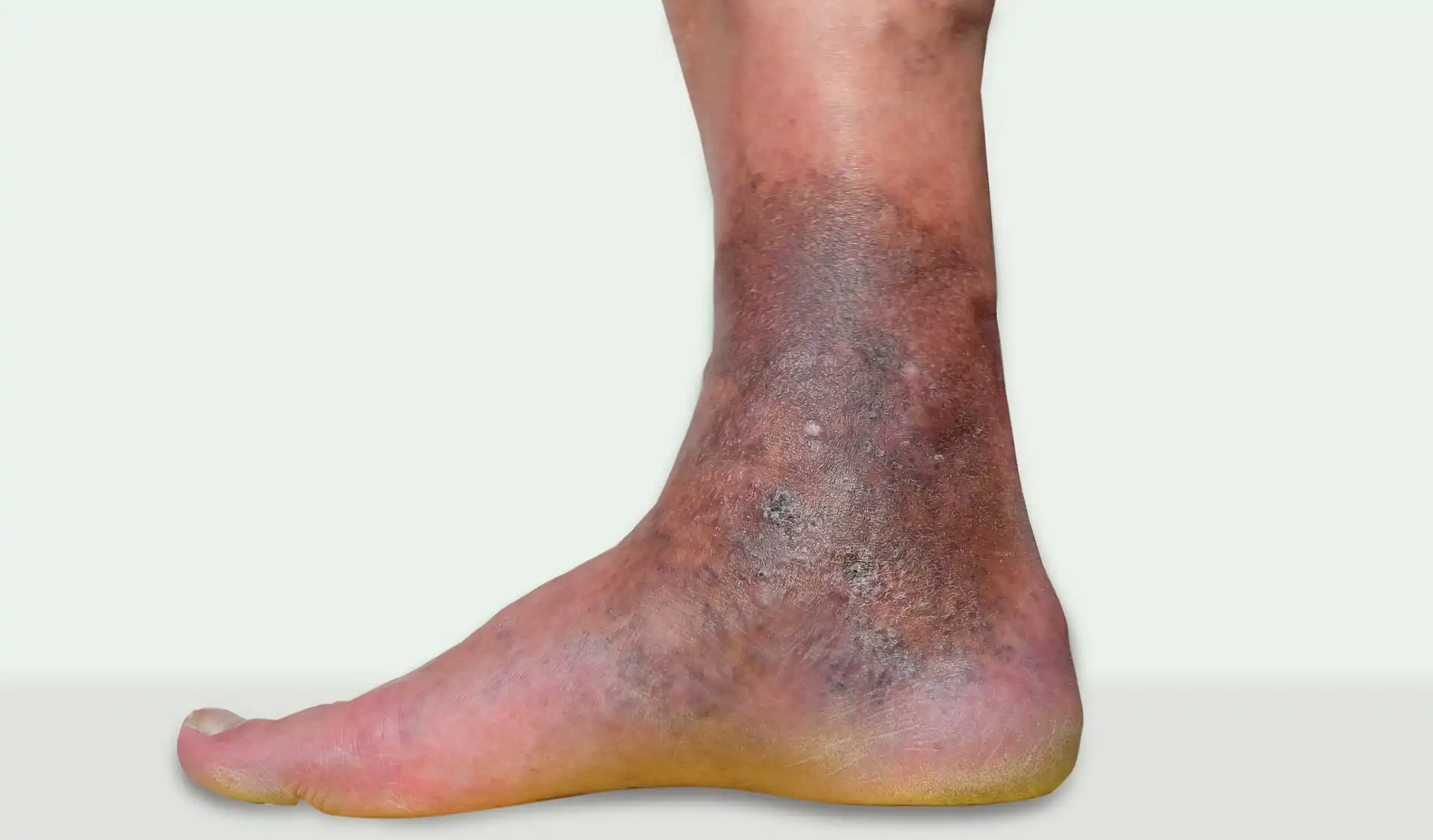

What is a Venous Leg Ulcer (VLU)?
A venous ulcer - also called a venous leg ulcer or stasis ulcer - is an open sore that develops on the lower leg or around the ankle when the veins can no longer return blood efficiently to the heart. Healthy veins rely on a series of one-way valves to push blood upward against gravity. When these valves weaken or become damaged, a condition called chronic venous insufficiency (CVI), blood pools in the lower limb, venous hypertension builds in the surrounding tissue, and the skin gradually breaks down into a wound that cannot heal on its own.
Venous ulcers account for the majority of all chronic leg wounds and are the most advanced stage of untreated venous reflux disease. They are most common in people over 50 but can affect anyone with underlying venous, arterial, or metabolic conditions. Critically, without correcting the diseased vein responsible for the blood reflux, even well-managed wounds are highly likely to recur.
Recognising the Symptoms: When Should You See a Vascular Surgeon?
Venous ulcers often develop gradually. The following early warning signs indicate progressive venous disease that will worsen without specialist intervention:
Persistent heaviness, aching, or throbbing in the lower leg
Swollen leg with a wound or swelling around the ankle, particularly after standing
Skin discolouration - brownish or reddish staining around the ankle
Hardening or thickening of the skin (lipodermatosclerosis)
Itching, scaling, or a weeping rash (varicose eczema) around the affected area
An open, shallow wound with irregular edges has not healed within 2 to 4 weeks
Causes and Risk Factors of Venous Ulcers
Damaged venous valves causing venous reflux & venous hypertension
A history of deep vein thrombosis (DVT) or post-thrombotic syndrome
Varicose veins - dilated, poorly functioning superficial veins
Superficial or deep venous insufficiency left untreated for years
Obesity, which places increased pressure on the venous system
Prolonged standing or sitting, which limits natural venous return
Diabetes and peripheral neuropathy, which impair wound healing
Arterial insufficiency that reduces oxygen delivery to the tissue
Advanced age, family history of vascular disease, or previous leg injury or trauma
One of the most common reasons a venous ulcer fails to heal or keeps coming back is that treatment focuses only on the wound surface - with dressings and compression - without ever correcting the faulty vein driving venous hypertension.
Treatment for Venous Ulcers By Dr Ravul Jindal
Effective venous ulcer care requires a two-pronged approach: healing the wound on the surface and correcting the underlying venous disease driving it.
Venous Recanalization
A minimally invasive, image-guided procedure restoring flow through blocked deep veins using balloon angioplasty or venous stenting to relieve hypertension and swelling.
Ulcer Management & Correction
Closes the faulty vein using laser, RFA, or VenaSeal while managing the wound with compression and advanced dressings to ensure lasting healing.
Preventing Recurrence
Wear graduated compression stockings as directed.
Maintain a healthy weight to reduce venous pressure.
Perform regular calf exercises to aid blood return.
Elevate legs during rest, especially after standing.
Manage comorbid conditions like diabetes and hypertension.
Avoid prolonged sitting or standing without movement.
Why Patients Across Punjab Choose Dr. Ravul Jindal for Venous Ulcer Treatment
Dr. Ravul Jindal combines international vascular training with 30+ years of surgical expertise, offering patients across Punjab access to advanced, precise, and personalised venous ulcer care.
- 30+ years of dedicated vascular and venous surgery experience.
- International training at St Mary's Hospital London, Imperial College.
- 16+ years as Director and HOD of Vascular Surgery, Fortis Mohali.
- Minimally invasive procedures with same-day or next-day recovery.
- Holistic care treating both the wound and underlying venous disease.
Advanced colour Doppler ultrasound and catheter labs ensure precise diagnosis - delivering effective, personalised venous ulcer treatment for every patient across Punjab and beyond.
4000+
Successful Surgeries
30 plus
Years Exp.

Frequently Asked Questions
Get expert answers to your concerns about venous ulcers, healing times, and advanced treatment options from Dr. Ravul Jindal.
What is the difference between a venous ulcer and a diabetic foot ulcer?
How long does a venous ulcer take to heal with proper treatment?
Is venous recanalization a surgical procedure?
Will my venous ulcer come back after treatment?
What is the best doctor to see for a venous ulcer in Mohali or Chandigarh?
Is laser ablation painful and what is recovery like?
Expert Vascular Care for Better Recovery
Get a specialist review for venous ulcer treatment in mohali - expert vascular care with personalised guidance and treatment planning.